Asking for an outbreak of preventable diseases
With vaccination rates plummeting, are anxious parents putting everyone at risk?
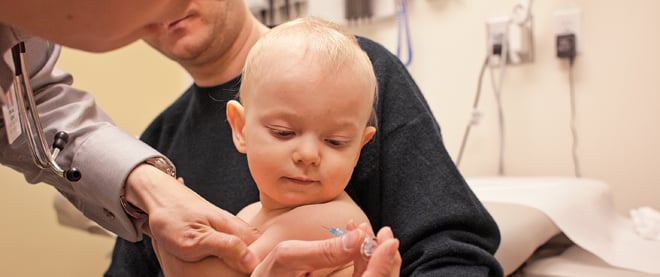
Photograph By Andrew Tolson
Share
On April 8, Pierre Lavallée took a call from Quebec’s public health office. Lavallée was into his fifth and last year as principal at Marie-Rivier high school in Drummondville, a town of about 67,000 an hour’s drive east of Montreal. He learned that a school employee had gone to the emergency room with a fever and rash the day before. Doctors quickly isolated the woman and rushed her to intensive care, where she was diagnosed with measles, a highly contagious and potentially deadly virus. According to the World Health Organization, measles was eradicated from the Americas in 2002.
Later, just after four o’clock, Lavallée received a fax from Dr. Danièle Samson, the director of infectious diseases for the region. “The staff and students at Marie-Rivier were in contact with a person very likely suffering from measles,” it began. The letter was to be forwarded to 1,475 students and staff, but most had already left for the weekend, so it was only circulated the following Monday. “I actually had measles when I was six or seven years old,” says Lavallée. “It was 40 years since I’d even heard of it popping up.”
Thus began what the Quebec government calls by far the worst measles outbreak in the Americas in 20 years. Over the next eight months, 763 cases were reported in the province, the vast majority in Mauricie and Centre-du-Quebec, a region that includes Drummondville. Roughly 11 per cent of those who were infected were hospitalized. Even a few who were inoculated as children caught the virus. “I didn’t think I could get it,” says Pascal Tarakdjian, 38, a science teacher at Marie-Rivier and the second confirmed case at the school. “I went to the hospital and told the staff that I might have measles symptoms, but they didn’t react because they didn’t know.”
Bracing themselves for another flood of cases this winter and spring, when measles infection rates tend to peak, officials are rolling out an immunization drive across Quebec, aiming to vaccinate 200,000 people. It’s necessary, they say, because falling coverage rates are to blame for the outbreak.
Since routine immunization began, infectious diseases that plagued us—measles, mumps, diphtheria, polio—have all but disappeared. For a growing number of people who haven’t seen them first-hand, anxiety about vaccines is replacing fear of the disease. Parents are increasingly delaying their kids’ shots, or cherry-picking certain vaccines and refusing others. A small, vocal minority avoids all vaccines, often out of the discredited belief that childhood immunization can cause autism. Young doctors are also more ambivalent about vaccines than their older peers. A survey of 551 U.S. doctors showed that recent medical school graduates were 15 per cent less likely to believe they were effective, suggesting the urgency around vaccination is fading away even among physicians.
Public health experts say that roughly 95 per cent of a population has to be vaccinated to provide what’s called “herd immunity,” the critical mass that stops a contagious disease in its tracks. As vaccination rates continue to fall, preventable diseases might start to reappear. “Measles is the one we’d expect to see first, because it’s so infectious,” says Dr. Kumanan Wilson, Canada Research Chair in public health policy at the Ottawa Hospital Research Institute, University of Ottawa. “Hopefully we will see this resolved before polio or worse emerge.”
Today in Canada, measles is extremely rare. In the last decade, the country typically saw less than a dozen cases per year, according to Dr. John Spika, director general of the Centre for Immunization and Respiratory Infectious Diseases at the Public Health Agency of Canada (PHAC); most were people who were infected abroad, then returned home. It makes Quebec’s massive outbreak particularly troubling. The province first started seeing a smattering of measles cases in early 2011, but they followed a typical pattern: travellers returning from other parts of the world, like France, where a measles epidemic has been raging since 2008 due to low vaccination rates. “We saw a few cases, and then they died out,” Spika says. “It wasn’t until April that it became self-sustained.”
In all likelihood, the Drummondville school employee unknowingly contracted measles in Montreal’s Trudeau Airport en route to a vacation in Cuba; the PHAC later analyzed the genetic makeup of the virus, and confirmed it to be the same strain circulating through France. It passed, as measles does, in the air—in this case, through the corridors and classrooms of Marie-Rivier.
Tarakdjian, feeling flashes of hot and cold, went to the emergency room with extreme flu-like symptoms on April 18. He’d shown the rash on his belly to a fellow teacher, who thought it might be measles (the first case had been diagnosed 10 days earlier, but there had only been one since). The hospital sent him home after seven hours in isolation with a burning fever, even though he hadn’t seen a doctor. He returned to work the next day. “I might have spread the virus at school,” he says. Tarakdjian left work the next day and went to a clinic with emergency services where he was diagnosed and spent the night in intensive care. The following two weeks, he vomited so much he couldn’t sleep. He didn’t return to work for four months because he was so exhausted and weak. The only one who had it worse was his colleague, the first woman infected, who, according to Tarakdjian, lost some hearing in one ear.
The situation at Marie-Rivier became dire enough that on May 25, school board commissioner Christiane Desbiens sent a voice mail to the parents of some 11,000 students in the district, urging them to make sure their kids were properly vaccinated. It’s very unusual for people who’ve been immunized to come down with measles, but it does happen, particularly among those who’ve received only one dose of the vaccine. (Provinces began to recommend a two-dose immunization schedule in the 1990s.) At the school, officials found, roughly four per cent of those who’d been vaccinated were felled by measles—but among the unvaccinated, the attack rate was much higher, and 82 per cent got sick.
Public health workers wondered what made this school susceptible. “Our hypothesis was that it had lower vaccination coverage rates compared to other regions,” says Dr. Horacio Arruda, the province’s director of public health (he would not identify Marie-Rivier as the school). In fact, Drummondville seemed fairly typical. “We were surprised to find that it didn’t differ too much from other schools across Quebec.” About 85 per cent of people at the school were immunized—lower than the 95 per cent health officials aim for—but not strikingly lower than schools elsewhere in the province, where vaccination rates vary from 63 to 93 per cent.
That picture continues across Canada. Only Ontario, New Brunswick, and Manitoba require that kids receive some vaccinations before attending school (all including measles), but even in those provinces, parents can opt out on medical or religious grounds, or simply for reasons of conscience. (Australia, by comparison, recently announced plans to withold tax benefits from families that refuse to vaccinate their kids.) In Canada, it’s hard to know for sure how good our coverage is, because no national tracking method exists. A public health information system called Panorama has been in the works for almost a decade now, which could follow vaccination uptake; until it becomes fully operational, vaccinations are tracked by public health agencies, physicians’ offices, and by patients themselves. (Quebec is planning to use the data it gathers as part of its current vaccination campaign to create a more effective province-wide registry.)
For now, we can only estimate coverage across Canada. The PHAC says that about 62 per cent of Canadian two-year-olds were up to date for all recommended vaccines in the most recent year they checked, 2009. It seems the measles outbreak at Marie-Rivier could have happened in countless other places—in some ways, it was just their bad luck.
When Jeanelle Robles’s son Makai was 2½ months old, she took him for his first checkup. “I thought it was best to listen to the pediatrician and get him vaccinated,” says Robles, 29, who lives in Toronto. “Before we saw the nurse, I felt hesitant. My baby was very little.” After Makai received his shots, he came down with a fever. “I slept with my baby, and he cried the whole night,” she says. Robles and her husband decided he wouldn’t get any more vaccines. “Medical intervention is necessary in so many situations,” she says. “But we’ve been brainwashed to think the only way to heal children is by medicine, antibiotics and vaccines.” Makai is now 3, and has a 10-month-old brother, Kaden, who hasn’t received any vaccines. “My friends ask, what would happen if he caught something?” she says. “And I say, what would happen if he caught something from the vaccine?”
Vaccines do carry potential risks. In a study of Ontario toddlers, Wilson found that about one in 168 who got the MMR shot (measles, mumps and rubella) at 12 months went to hospital between four and 12 days afterwards. Most had fever and other viral symptoms, but few were sick enough to be hospitalized. After receiving the MMR vaccine, about one in a million patients will develop encephalitis, a potentially fatal inflammation of the brain. But about one in 1,000 patients with measles will develop encephalitis, a much higher rate. (No encephalitis cases or deaths from measles were reported in Quebec as of December.)
Former Playboy model Jenny McCarthy has blamed the MMR vaccine for causing her son’s autism. A supposed link between the two was implied in a 1998 scientific study published in The Lancet, sparking a massive scare; in 2011, its author, Andrew Wakefield, was declared a fraud. Wakefield’s paper was retracted, and he was disbarred from the practice of medicine, but the damage was done. Fear of autism remains one of the top reasons that parents refuse or defer vaccinations, according to a U.S. survey.
“People who are concerned about vaccine safety issues are looking at a collapse in children’s health,” says Edda West, coordinator of the Vaccination Risk Awareness Network (VRAN), which has about 500 members across Canada, including Robles. In a statement, she cited “the explosion of autism spectrum disorders, learning disabilities, ADHD, allergic and anaphylactic disorders, asthma, neuroimmune and autoimmune disorders and other chronic diseases that parallel the steep rise in numbers of vaccines injected into infants and young children since the 1980s.” West believes that health officials have yet to produce long-term studies, “free of conflicts of interest,” comparing the overall health of unvaccinated and fully vaccinated kids. Until then, her statement adds, they can “continue to deny the real cost aggressive vaccine schedules extract from the public health.”
A little over a decade ago, undervaccinated kids were more likely to come from families that had trouble accessing health care, or from strict religious communities that forbade the practice. Today’s unvaccinated children are “more likely to be white, to belong to households with higher income, [and] to have a married mother with a college education,” says a 2009 study in the New England Journal of Medicine, which notes that parents of unvaccinated kids are more likely to seek alternative health care, and to use the Internet as an information source.
They also tend to live close to one another—maybe drawn together by an alternative school, church or politician, or to live near like-minded neighbours—which creates vulnerable pockets across the country. Beyond the financial cost of an outbreak, it puts others at risk, like babies too young to be immunized, those who can’t be vaccinated for health reasons, and people like Tarakdjian.
If vaccination rates dip too low, the consequences will be serious for everyone. In 2010, the Canadian Medical Association Journal (CMAJ) published an editorial flagging a polio outbreak in Tajikistan, which was certified polio-free in 2002. That country may not seem to have much in common with Canada; but with an 87 per cent uptake of the polio vaccine, its rate is actually quite close to some Canadian regions. (The WHO recommends a minimum of 90 per cent coverage.) “This dreadful disease has no cure and causes paralysis and even death,” the editorial states, noting that Tajikistan’s outbreak should be “clanging alarm bells. We are only one asymptomatic infected traveller away from an outbreak because of low vaccination rates.”
At a doctor’s office in St. Michael’s Hospital in downtown Toronto, Paul Bradshaw bounced his 16-month-old son Sam on his knee. “Come on, show us your muscles,” Bradshaw said, as Dr. Fok-Han Leung prepared to give the toddler a flu shot. When the needle went in his arm, Sam turned his face into his father’s chest for comfort, but didn’t shed a tear. After a bandage was applied, he was running around the room again, clapping his hands together, until it was time to go. “It needs to be done,” Bradshaw says. “If he got an illness because we missed a vaccine, I would feel awful. Besides,” he says, “nobody in our house sleeps when Sam’s ill.”
In Quebec, doctors, nurses, and public health workers are crossing their fingers that most parents and young adults will feel the same way as Bradshaw. Until a powerful reminder resurfaces, it’s easy to forget the consequences of missed vaccines. “We are happy we haven’t seen anybody who died or got encephalitis,” Arruda says. “It’s not acceptable to be worrying, in the year 2012, about these preventable diseases.”