Is it right for doctors to deny patients unproven anti-COVID-19 therapies?
Dr. Raiyan Chowdhury: The coronavirus crisis is a threat that needs urgent answers, but those answers cannot come fast enough for those who are sick right now
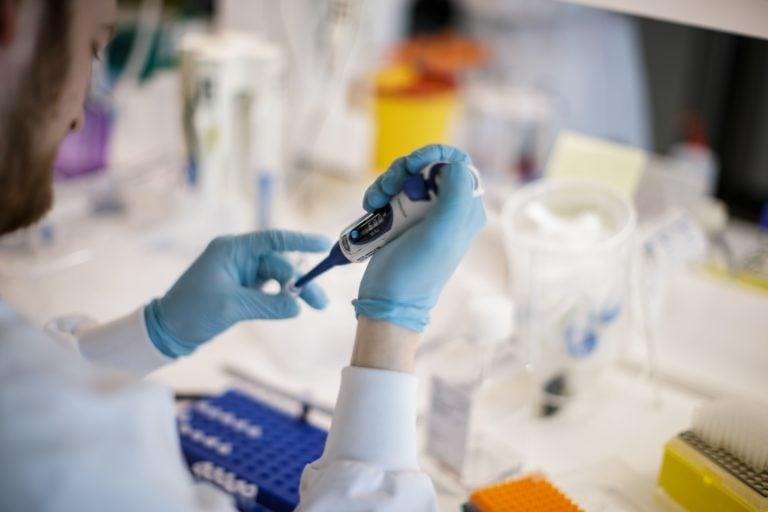
A researcher works on a COVID-19 vaccine at Copenhagen’s University research lab in Copenhagen, Denmark, on March 23, 2020 (THIBAULT SAVARY/AFP via Getty Images)
Share
Dr. Raiyan Chowdhury is a critical care medicine specialist and an ENT surgeon, with research focus in Health Quality / Patient Safety at the Royal Alex ICU, a 30 bed tertiary care unit in Edmonton, and an assistant professor at the University of Alberta.
Throughout Canada, potential therapies against COVID-19 are being limited to only patients enrolled in clinical trials. For doctors and nurses treating COVID-19 patients, the question and moral dilemma of what to do with unproven therapies lingers. Should patients have a right to these unproven therapies?
U.S. President Donal Trump has outspokenly advocated for the use of hydroxychloroquine and azithromycin. Juxtaposed to his enthusiasm, institutions and organizations in Canada have urged against the use of such medications outside of well regulated, scientifically rigorous clinical trials. The Public Health Agency of Canada and the Canadian Critical Care Society released statements suggesting the use of investigational anti-COVID-19 therapeutics should be limited to ethically approved, randomized, controlled trials.
One of the bright lights that arises from this human suffering is the once-in-a-generation sharing of the human experience. Canadians are more empathetic these days. I find myself more appreciative of my grocery store clerk who now finds herself on the frontlines. The store’s freshly baked banana bread was a good break before our worlds suddenly changed. But now, I find it even more comforting. Everyone has some example of this. We probably feel the greatest empathy for the physicians and nurses who are serving in the hardest hit areas. Despite their daily struggle, health care providers from places like Lombardy and New York City have shared clinical pearls and advice in real time. Peer reviewed publications with appropriate scrutiny will eventually follow, but they realize their advice is needed now. Those elsewhere are probably indebted. Our patients deserve this same empathy and flexibility now.
READ MORE: Coronavirus in Canada: These charts show how our fight to ‘flatten the curve’ is going
As intensive care medicine physicians and nurses, we are the last line of human intervention between what separates life and what lies beyond. Our therapies and interventions are guided by evidence-based medicine comparing the effectiveness or harm of different therapies. Combined with our own prior experiences or intuition with a given treatment, we provide guidance to our patients on what we think is best.
While we heavily rely on evidence, we also understand that individual patients are unique and do not necessarily fit nor qualify for the homogeneity attempted in trials. Our profession as intensivists is as much science as it is art.
Rigorous studies looking at anti-COVID-19 therapies are not yet completed. The disease itself first appeared in late December and much of the western world, including Canada, probably didn’t take it seriously until March. This is hardly enough time to produce detailed observational studies, let alone randomized controlled trials.
Initial papers are at least now being published. The WHO has subsequently started its multicentre randomized controlled trial named Solidarity, looking at the effectiveness of therapies including the anti-malarial hydroxychloroquine, the anti-viral remdesivir, and HIV medications lopinavir/ritonavir.
One day, we will have a vaccine. There are simply too many people smarter than you and me working on this for that not to happen. There will eventually be some degree of herd immunity, and social distancing will flatten the curve. B.C. and Alberta are already reporting evidence of this flattening. Randomized controlled trials will eventually be published showing the benefits or harms to the above therapies. These publications will of course be too late for those who have critical COVID-19 illness now.
In mid March, my younger brother, who is also a physician, was diagnosed with COVID-19. He acquired the illness at the hospital. About 5 days after he first noticed symptoms and had already tested positive, his conditioned worsened. He went to the emergency feeling short of breath and tightness in his chest.
We both discussed additional potential therapies if his condition worsened. While his clinical case eventually improved without further therapies, the experience left me with a greater empathy for Canadians whose experience with the illness has not been as fortunate. When you are on the other side of COVID-19, therapeutics that are called “unproven” and “experimental” may be better termed “hope.”
In the early seasons of Grey’s Anatomy, the Fray’s “How to save a life” became an unofficial theme song for the show. The lyrics “Let him know that you know best, cause after all, you do know best” always seemed to stand out at me. As doctors and nurses, we hope we know best. We must equally recognize when we don’t. When it comes to anti-COVID-19 therapies, nobody yet knows their benefits and harms in that context. True clinical equipoise exists.
“First, do no harm.” Some physicians and nurses may feel strongly against the use of these unproven therapies. I can understand the reasoning. Any of us who have practiced medicine and intensive care long enough have seen countless therapies that promised the world, only to find through detailed studies that they were helping kill our patients.
At the same time, some of us are critically aware of the shortcomings of modern medical research. Over the years, a variety of therapies proven to promise mortality benefit in initial studies—activated protein C, tight glycemic control, early goal directed therapy—significantly changed clinical practice, only to be later abandoned when subsequent studies showed no benefit and often harm.
Despite all the rigours of modern experimental design, our field is still susceptible to cultural, social, economic and moral biases. Much of what we do in ICU is based on possible physiological benefit rather than demonstrated evidence. Once in ICU, given that the alternative is death, all intensivists have at some point offered therapies that lacked evidence. The reason for that is simple. Not everything in medicine can be studied and distilled into an RCT. Physicians who may be unwilling to offer anti-COVID-19 therapies for those who are critically ill are at risk of being inconsistent.
If potential anti-COVID-19 therapies are currently denied outside of research trials, only to be proven effective by trials a few months later, we risk a disservice to our patients. One that may cost lives. Such policies also risk principles of equality and universal access. Patients in places as varied as Red Deer and Thunder Bay will not have the same access to potential therapies as patients in Toronto, where academic centres are plenty.
Training as a physician instills that an organized approach is needed when it comes to a public health crisis. We need organized social distancing, reasoned rationing of PPE, and appropriate use of ICU resources. We of course need well organized, scientifically rigorous studies of the use of these medications. There is no denying that. Therapy, however, should never be a one-way street.
There is a reason why the Institute of Medicine equally balances patient safety and patient centredness. It is a mutual road of give and take—one that balances a patient’s wishes / values and the evidence base /experience of health-care providers.
This crisis requires us to be flexible. We face a threat that needs urgent answers, but those answers cannot come fast enough, particularly for those who are sick now. Blanket avoidance of the use of unproven therapies outside of trials may not be the right answer. Our patients and the public should at least have a say.