Fighting scary vaccine stories with scarier no-vaccine stories
Skepticism over shots is making doctors more PR savvy
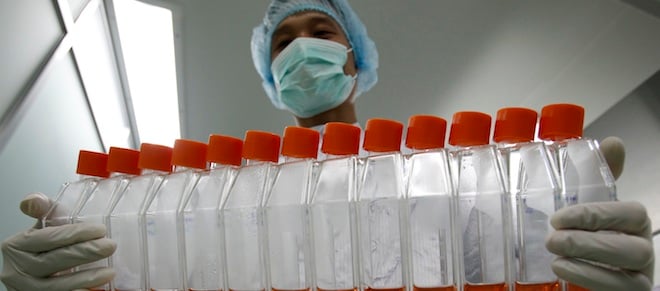
Researcher Hoang Duc Loc carries containers of dengue virus titration assay at a cell culture laboratory of Vietnam’s Vabiotech on dengue fever research in Hanoi June 6, 2012. One of the grimmest legacies of the war in the Pacific is still being fought 70 years on, but a victory over dengue, the intensely painful “breakbone fever” which that conflict helped spread around the world, may be in sight. REUTERS/Kham (VIETNAM – Tags: HEALTH SCIENCE TECHNOLOGY)
Share
People hate getting vaccines. Apparently even vaccinologists.
“I don’t like to get immunized,” Science-ish was surprised to hear from one of Canada’s most esteemed vaccine researchers this week. “I do, and I will continue, but I put it in the same category as going for a colonoscopy.”
With the re-emergence of diseases like measles and whooping cough, and parents increasingly seeking alternative vaccination schedules or opting out of shots all together, policymakers are scrambling to figure out what to do. In California, for example, the state legislature is now looking at a bill that would require parents who want to decline vaccines for their kids to seek counseling from a doctor.
Here in Canada, some hospitals have begun essentially forcing health-care workers to get the flu shot if they want to keep their jobs. We’ll never see that kind of measure applied to the general population, so for now: What do we know about what works when it comes to getting people to comply with vaccine guidelines?
Surprisingly little. Those who research these issues—including the vaccine-hating vaccinologist Dr. Andrew Potter—told Science-ish we have no good evidence on interventions that get refusers to change their minds. Part of the problem, of course, is that it would be difficult to find vaccine-shy people who would participate in a study on how to get them to enroll in an immunization program. The other issue, said Mayo Clinic infectious diseases expert Dr. Gregory Poland, is that vaccine denial “is a relatively new phenomenon.” Though there was opposition to vaccination in the 19th and 20th centuries, “From post-WWII up until about the early 1990s, no one really rejected vaccines.” So the science simply hasn’t caught up.
For now, we can run pilots, as California is thinking of doing, and see what works to boost coverage. But Dr. Poland, and others Science-ish spoke to, think a program like the Golden State’s is unlikely to improve uptake since it assumes more education will lead to better coverage. And we already know that’s not always the case. “People who make a decision to reject vaccines are making a decision based on anecdotes, misrepresentation, fear, and emotion,” he said, citing examples of communities like Vashon Island in Washingston State. There, despite the relatively high levels of education, access to health care, and wealth, large swathes of the population refuse to vaccinate their kids against childhood diseases.
Scientist and author Michael Shermer has coined a phrase for the kind of anecdote-driven decision-making that seems to shape choices like rejecting vaccines. He calls it belief-dependent realism. This is when people make decisions, and then accept or reject the evidence on a given issue based on whether it validates their decisions. That seems to be one reason why parents wind up exposing their children to the one in one thousand chance they will get a disease that would be managed with vaccination, instead of the one in ten million chance a vaccine could make them sick. (Science-ish won’t delve into already well-debunked vaccine myths, so see here or the open-access version here for a summary.)
“Both [getting vaccinated and refusing to do so] have a risk, both have a benefit. By reasoning, you’d see that the vaccine offers the most benefit and the least risk,” said Dr. Poland. Still, stirring, cherry-picked anecdotes of the very rare or non-existent side-effects of vaccines—spread by the likes of Playboy model Jenny McCarthy or the now-infamous researcher Andrew Wakefield—have a powerful hold on people’s minds. Education or good data may not necessarily have any impact on those folks.
However, Dr. Poland suggested, “One way to reach them is with emotional appeals.” When he confronts anti-vax parents at the Mayo Clinic, he brings out his own scary anecdotes: photos of babies with a particular vaccine-preventable disease, or video testimonials from parents who lost a child as a result of refusing to immunize. “It’s fighting emotion with emotion and it harkens to the fact that—if you’re somebody whose decision model is emotional—wisdom resides with me discussing this on the level at which you make decisions.”
Science-ish is a joint project of Maclean’s, the Medical Post and the McMaster Health Forum. Julia Belluz is the associate editor at the Medical Post. Got a tip? Seen something that’s Science-ish? Message her at [email protected] or on Twitter @juliaoftoronto