Why people hooked on opioids, especially in the U.S., keep falling through the cracks
The author notes that the culture of pill-taking often takes hold in early life, when kids are prescribed drugs such as Adderall or Ritalin for ADHD
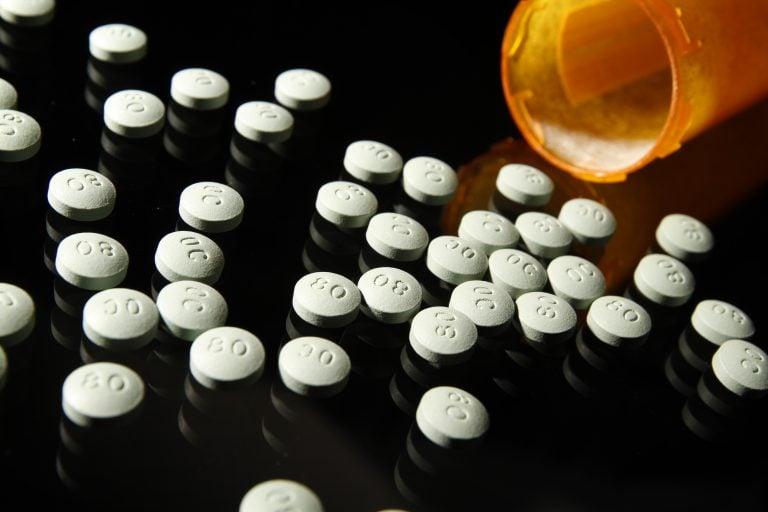
OxyContin 80 mg pills. (Liz O. Baylen/Los Angeles Times via Getty Images)
Share
As Beth Macy wrote her new book, Dopesick, about the opioid crisis in the United States, she felt a weight of responsibility—to the mothers of the addicts whose stories she was telling, to the first responders who were helping with overdoses or confronting dealers, and even to those working in the overburdened legal system. She relates what a drug court judge told her: “‘I can’t wait to read your book, because then maybe we’ll know what to do’—but he seemed closer to tears than laughter.”
The Roanoke, Va.-based writer tasked herself with unravelling a demonically complex issue, and Dopesick is both devastating and sprawling in scope. In part, it’s a David-versus-Goliath narrative like her first book, Factory Man (2014), which details a Virginia furniture business’s fight to save local manufacturing jobs in the face of competition from China. Early in Dopesick, we meet activists from what Macy calls “sentinel communities” in Virginia, which suffered the dreadful effects of opioid addiction soon after OxyContin was introduced in 1996. They resolved to take on pain-management behemoth Purdue Pharma, which aggressively marketed its drug.
Despite the company’s $634-million (U.S.) settlement in 2007 for “misbranding” OxyContin as resistant to abuse, the battle is still being fought. “You can see so many parallels [between] what was happening in rural Virginia in the late ’90s and what’s happening now,” says Macy. “People walking around with smudges on their shirts because they’d figured out how to get the time-release coating off the pills to get the full bump of the euphoria, and people being killed because they’re making night deposits at the bank, by addicted people so desperate to get these drugs that they’re willing to murder for it.” An estimated 2.6 million people in the U.S. have opioid-use disorder, while in Canada, close to 4,000 people died of opioid overdoses in 2017; a poll this year found that one in eight Canadians knows that a family member or a close friend is addicted.
READ MORE: Trump declared the opioid crisis an emergency. Why won’t Trudeau?
In Dopesick, Macy interweaves the stories of those in distressed communities across Appalachia who have promoted, prescribed, dealt, been addicted to, and fought the spread of opioids—as well as those who treat addiction. She spoke with Maclean’s about how opioids took hold, and what might be done to loosen their grip.
Q: As you researched the historical trajectory of the opioid crisis, did you find there was a time when it seemed the problem might reasonably have been contained?
A: Yeah, in the U.S. Attorney’s office, that plea agreement in ’07 was pronounced a huge victory. And as we see in the book, because of Rudy Giuliani’s efforts to minimize the government’s case [Giuliani was hired as a consultant by Purdue Pharma], he also minimized the impact of the punishment, so [parent company] Purdue Frederick gets [banned from Medicaid], not Purdue Pharma, and OxyContin goes on being widely prescribed. The prosecutors who worked that case now say, “Our hope was that the media attention would make doctors and patients leery of this drug,” but as late as 2015, we had Purdue Pharma officials saying to doctors in Richmond, Va., “What’s getting lost here is under-treated pain.”
They’re still out there promoting it, and in the developing world now, [there’s] this notion that pain is being under-treated when, 100 years before, people were so careful only to use [opiates] for cancer pain and end of life. Purdue Pharma nationalized the supply of opioids and, using false data, made doctors comfortable with the notion that opioids weren’t addictive. You also had a very complicit FDA allowing Purdue to make the claim that [OxyContin] was believed to reduce the liability of abuse, even though no long-term studies had been made. And in effect, Purdue’s own studies showed that you could recover 68 per cent of the oxycodone in OxyContin in one bump, if you took the coating off [a pill] and crushed it and injected it. Where was the FDA oversight?
Q: You write about doctors being given “Oxy”-branded beach hats, as well as junkets and free meals. It’s shocking to what degree prescribing the drug was incentivized.
A: I was a newspaper reporter for 25 years, and we were always told you can’t take a lunch that’s worth more than $25, and yet 5,000 doctors, pharmacists, and nurses went on free trips to pain-management seminars. Studies show they came back and wrote twice as many OxyContin prescriptions. Where were the ethics? Recently I was invited to address a group of medical professionals, and I said, “I feel like any doctor who ever accepted a freebie from a pharmaceutical company should feel morally compelled to get waivers to prescribe medication for the treatment for addiction,” and they just looked at me—you could have heard crickets. The moderator, who was a physician, cut me off and went on to the next person on the panel. There’s so much lack of responsibility everywhere you look in this epidemic.
Q: One significant problem you address is the ongoing debate about treatment: whether it’s best to go cold turkey from opioids or wean people off with related drugs.
A: Study after study shows that addicted people who use medication-assisted treatment—Buprenorphine and Methadone in particular—reduce their chances of overdose by more than half. Often people will send their children off to treatment, and when they get out, most relapse, and at that point, they’re opioid-naïve, and many go back to using the same amounts that they used before, and they die. [Buprenorphine] is not a perfect drug; clearly it doesn’t work for everybody, but it is the best protective thing. If our goal in public health is to prevent death, then this is a “low-hanging-fruit” way to do that. We know this works, so why aren’t we making it easier for people to get? I think Canada is doing a much better job with providing low-threshold access.
Q: Your book spells out how difficult it can be for someone to move from one stage of treatment to the next, for instance from the hospital to rehab. To what extent is this a medical-insurance problem in the States?
A: Oh, it’s huge, and it depends so much where you are. If you’re in Boston, you can go into a homeless shelter and be connected to somebody that’s going to help you get on extended Medicaid under the Affordable Care Act. You can be connected to a free MAT [Medication-Assisted Treatment] program. In Virginia, not so much. Virginia just passed the Medicaid expansion, and it hasn’t even officially filtered down to communities yet—and there are still 17 states that haven’t passed it.
People living on the streets need help accessing these services. When [one deceased addict’s] mom and I went out to retrace her [daughter’s] final steps a couple months ago, we went to the house of a friend of hers who had gotten some mail for her, because she was homeless. After she died, she had gotten a letter from the state of Nevada saying she had been approved for Medicaid. Even though she was living on the street and didn’t have an ID, she still figured out how to get access to medical care; it just didn’t trickle down to her fast enough. And when her mom opened that envelope up and saw her daughter’s Medicaid card, she burst into tears. She had held it together the whole week we were there. She said, “She’s trying so hard, and everything’s stacked against her.” We’ve just written these people off as a society—we helped them get addicted by providing opioid after opioid, but the moment they get addicted, we have no sense of urgency about getting them treatment for their addiction.

Q: In Dopesick, you cover how those who can’t easily obtain prescription opioids sometimes turn to heroin, and you interview one former dealer, Ronny Jones, who comes from a family with its own addiction problems. Still, he insulates himself from the devastation wreaked by his drug-dealing.
Right—he’s far from the point where the needle meets the vein. He has justified it in his mind, that he was actually making it safe, that people didn’t have to drive to Baltimore from the little farm town [of Woodstock, Va.] anymore to get their heroin, and he’s charging them less. He also doesn’t see that he’s complicit, like the pharmaceutical companies that claim they don’t understand how they’re complicit. So Trump blames Obama cutting back on imprisoning non-violent drug offenders but never makes a mention of doctors or pharmaceutical companies’ role, and it’s both. It’s everything.
Jones knew he would get caught eventually; according to many people, he tried to go legit [after leaving prison] and just couldn’t get a job. And his probation officer had 100 people on her rolls and couldn’t keep up with him. He had no way to get food stamps, and in order to pay his bills, he felt he had to go back to the only thing he knew that had provided him money. And by the time he got out from his second prison stint, the drug of choice in his community was opioids. He didn’t even know how to break heroin down; he had to hire some underlings. He was scared to death of “herr-on,” as he called it.
Q: These stories dovetail perversely with the ideology of American capitalism. Jones is making money as an entrepreneur providing a service that’s in theory cheaper and safer for people than existing ones. Big Pharma is seen to be providing a service, too, and of course it’s their right to make money…
A: Right, this behaviour [exists] at every turn—and even goes back to the CEOs closing the factories, so they can make more money if they have the product made in Mexico or in China. There are so many interweaving narratives.
READ MORE: The inside story of Canada’s opioid crisis
Q: What’s more, you write about the culture of pill-taking that takes hold often in early life, when kids are prescribed drugs such as Adderall or Ritalin, and how it’s easy to get from that into recreational pill-taking because you’re so used to taking pills all the time.
A: I happened to notice that everyone I was interviewing who had a problem with opioid addiction had started out with ADHD medication, whether it was prescribed to them or not. Kids who started taking it when they were young begin trading it in high school for harder drugs. A lot of kids in college want to take it so they can stay up all night drinking without passing out, and it becomes a currency. Anna Lembke’s book, Drug Dealer, MD, goes into more detail. The science isn’t clear; some people think that undiagnosed ADHD can lead to substance abuse disorder. I think it is clear that ADHD has been way over-diagnosed and certainly over-treated.
Q: Do you have any hope that there’s a meaningful political response gathering to opioid addiction, rather than just hot air?
A: Unfortunately, [addiction is] normal for families of all income levels and political stripes. We’ve got to pay attention. Trump promised he would declare a national emergency, and then he declared a public health emergency, which sounds like a national emergency but releases no new funds or authority. We’ve got to continue to hold our leaders accountable. Trump gave a lot of lip service to this, but Jeff Sessions’ [announcement about] executing dealers was lacking a lot. If you look at the dealers in my book, they’re tree-trimmers, they’re waitresses, former cheerleaders and high school football stars, and it’s just so much more complicated, because so many people who use also deal. The system is so tilted towards prosecutors: a lot of people that get caught dealing drugs lie to reduce their time, and it’s really a complex problem.
Q: You write about people who put in enormous effort to get helpful initiatives off the ground. It seems the system is stacked against anyone who wants to do anything differently.
A: Yes. And I knew the only way I could emotionally stand to spend two years on the subject was to focus on the people fighting back. Like Mr. Rogers said, “Find the helpers.” What I saw, over and over, was caregiver burnout in the families and the first responders. They’re working day and night, rescuing people out of drug houses, and you see MAT doctors overworked because not enough other doctors are willing to become waivered to prescribe MAT. To me, they’re the real heroes in this book.
I do see hope in these amazing people still hanging in there. Right now, [people with addiction] are falling through the cracks, and that’s why they’re ending up in this world of criminal gangs—women especially being trafficked and prostituted—or just left to fend for themselves. I think we’re going to gradually come to see treating people with addictions become one of the new civil rights frontiers—treating humans as patients worthy of medical care.
MORE ABOUT OPIOIDS:
- Health Canada’s latest weapon in the opioid wars: big yellow stickers
- How opioid vending machines could fix Vancouver’s drug crisis
- Learning to fight the opioid crisis at Vancouver Community College
- Facing the opioid crisis, an establishment doctor heads to the streets
- ‘Unexplained losses’ of opioids on the rise in Canadian hospitals