Will cancer screening actually save your life?
Science-ish looks at the evidence on PSA testing, mammograms and the true benefits of screening
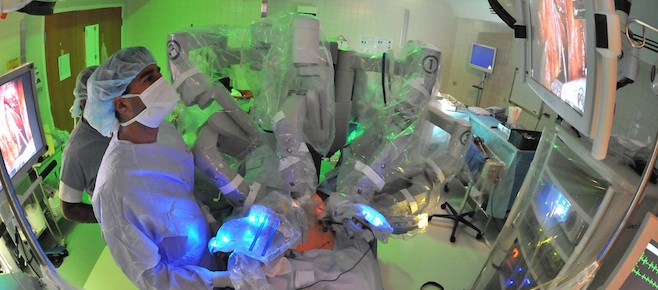
In this Sept. 13, 2011 photo provided by the University of Chicago Medical Center, Dr. Gautam Jayram assists during prostate cancer surgery, watching an internal video of the patientâs body, at the University of Chicago Medical Center in Chicago. No major medical group recommends routine PSA (prostate-specific antigen) blood tests to check men for prostate cancer, and now a government panel is saying they do more harm than good and healthy men should no longer receive the tests as part of routine cancer screening. The recommendation by the U.S. Preventive Services Task Force, being made public on Friday, Oct. 7, 2011 will not come as a surprise to cancer specialists. The task force concluded there’s little if any mortality benefit. But there is harm from routine screening: impotence, incontinence, infections, even death that can come from the biopsies, surgery and radiation, according to Dr. Virginia Moyer of the Baylor College of Medicine, who heads the task force. (AP Photo/University of Chicago Medical Center, Bruce Powell)
Share
“There is a powerful narrative among support groups and cancer survivors: Screening saves lives. . . For the most part, it’s wishful thinking. And it demonstrates the growing gap between what screening (and science more generally) can offer, and what the risk-averse public wants it to be.”—Globe and Mail, May 21, 2012
A recent recommendation by a U.S. government advisory panel to ditch the PSA test for prostate cancer has reignited the call for a cancer screening rethink. It’s no longer okay to abide by the “screen early, screen everybody” maxim, the conversation goes, echoing the one that emerged when the frequency of routine screening for breast cancer was scaled back last year.
Now, it’s good to be having these discussions: We do need to change how we think about cancer screening. In recent years, with the advent of incredible technologies that detect diseases before we feel sick, we’ve seen the emergence of “overdiagnosis.” The term describes cancer that is diagnosed but would not necessarily cause death or even symptoms because the cancer never grows, it regresses, or it spreads so slowly, the person dies before knowing any harm. That’s right, not all cancers are deadly or even harmful. As well, every single body displays at least a couple of benign abnormalities that can be seen as trouble. This is why mass screening has the potential to “rapidly turn perfectly healthy people into patients,” says the Canadian health policy researcher and author of Seeking Sickness, Alan Cassels.
Science-ish, though, wondered whether PSA testing and mammograms—usually the inspirations for the anti-screening cri de coeur because they can lead to overdiagnosis and unnecessary surgeries—are the exceptions in cancer screening or the rule.
According to Dr. Gilbert Welch, who has studied and written books on the problems created by early disease detection, breast and prostate screening are not alone. Mass screening has led to overdiagnosis in kidney, thyroid, and lung cancers, as well as renal cell carcinoma and melanoma. In one interesting case study in Japan, researchers did spiral CT screening in a community and found ten times as much lung cancer as they had previously detected in the same population using chest x-rays. “The really amazing part,” said Welch, “was that they found the same rate of cancer in smokers as non-smokers.” Since we know there’s a much greater risk of smokers dying from lung cancer than non-smokers, Welch explained, “This woke everybody up to the problem that there are a lot of cancers in the lungs that don’t go on to cause problems.” So early detection in these cases would have led to unnecessary treatment and stress.
Then there’s the contentious cancer survivor mythology. “The survivor has been seen as someone who has undoubtedly benefited from treatment for cancer,” said Welch. But the evidence shows many supposed “survivors” would have lived on anyways—because they didn’t need treatment to begin with. Welch’s Archives of Internal Medicine study on whether a woman with screen-detected breast cancer is likely to have had her life saved by treatment concluded that in most cases the answer was “no.”
That’s not to say, though, that all cancer screening is ineffective. Colorectal screening has been shown to dramatically save lives as a result of early detection, and the Pap test turned cervical cancer into a largely curable disease. Even mammograms and PSA testing—the poster children for overdiagnosis—find cancers in people who would have otherwise died from them. That’s the screening paradox. “Screening can both help people and hurt people at the same time,” Welch said. “It’s not one or the other.” Or, as Siddhartha Mukherjee put in his biography of cancer, The Emperor of All Maladies, “The trouble is that overdiagnosis and underdiagnosis are often intrinsically conjoined, locked perpetually on two ends of a seesaw.”
So where does this leave patients and their doctors? “We need to understand that cancer is not one disease,” University of Manitoba professor Alan Katz told Science-ish. “All cancers are different and we need to look at each one separately.” This means patients should ask about their individual risk of developing a particular disease—based on their medical history, age, risk factors, and symptoms—and how those weigh against the benefits of screening. For example, a young woman with no history of breast cancer in her family, and no risk factors or symptoms, can probably avoid getting screened until later in life, as both U.S. and Canadian guidelines suggest.
This flip flopping can undoubtedly be worrisome and confusing. But such is the reality of evolving science. PSA testing, like mammograms, once seemed to benefit more people than it harmed, but now the evidence suggests otherwise. As Welch put it: “The power of our technology to detect abnormality now far exceeds our knowledge of what we should do about it and in many cases the right answer is nothing.”
Science-ish is a joint project of Maclean’s, the Medical Post and the McMaster Health Forum. Julia Belluz is the associate editor at the Medical Post. Got a tip? Seen something that’s Science-ish? Message her at [email protected] or on Twitter @juliaoftoronto