Opioid crisis: Trump declared it an emergency, why won’t Trudeau?
Opinion: By declaring a national public welfare emergency, Ottawa could unlock critical funds to respond to Canada’s opioid crisis
A woman carries a naloxone kit and a bag from Insite, the safe injection site, while walking in the Downtown Eastside of Vancouver, B.C., on Wednesday July 27, 2016. Naloxone is used to reverse the effects of overdoses in drug users who have taken opioids. The provincial government has announced the creation of a joint task force on overdose response. (Darryl Dyck/CP)
Share

Pauline Voon is a research associate at the BC Centre on Substance Use and doctoral candidate in population and public health at the University of British Columbia. This piece originally appeared at The Conversation.
In the United States, President Donald Trump has formally declared the opioid overdose crisis to be a national public health emergency. The numbers he cited speak for themselves: More than 64,000 Americans died from opioid overdose last year, which translates to more than 175 per day, or almost seven every hour.
The situation in Canada is just as devastating, with opioid overdoses estimated to cause at least 16 hospitalizations and eight deaths each day.
This did not happen overnight. The number of opioid overdose deaths has risen at an alarming rate since the early 2000s. Now, more than a decade later, communities, health professionals and some politicians such as NDP Leader Jagmeet Singh, are still pushing for a national health emergency to be declared here in Canada as well.
By declaring a national public welfare emergency, the federal government could both acknowledge the scale of the opioid overdose crisis and unlock funds critical to a successful response.
Such a move would not be without precedent.
From SARS and H1N1 to opioid deaths
We should have learned by now, from past health crises that have affected our entire nation.
When 44 deaths were caused by SARS in Canada in 2003, the National Advisory Committee on SARS and Public Health urged the Government of Canada to “consider incorporating in legislation a mechanism for dealing with health emergencies” — one that “would be activated in lockstep with provincial emergency acts in the event of a pan-Canadian health emergency.”
In 2009, when 428 deaths were caused by the H1N1 flu virus in Canada, an Emergency Operations Centre was mobilized 24 hours a day, seven days a week for several weeks. This provided more than 6,000 person-days of manpower to help coordinate emergency responses across the country.
In comparison, only 113 person-days of assistance for the opioid crisis have been reported by the Public Health Agency of Canada — to help write reports in two jurisdictions last year — despite more than 2,800 deaths from opioid overdoses in 2016 alone.
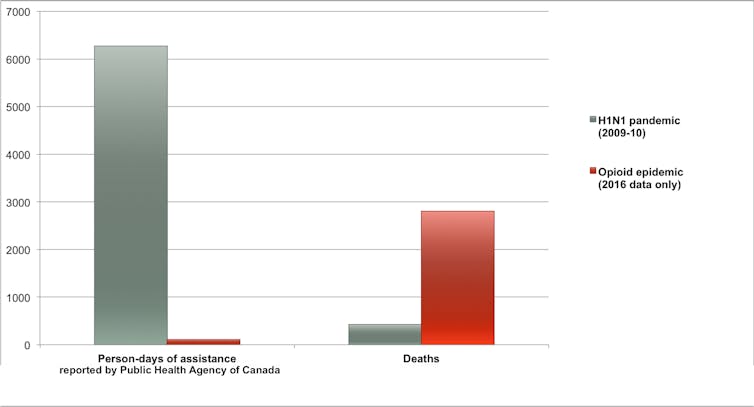
Author provided
The federal government has already implemented important measures, such as improving access to life-saving treatments and approving supervised injection sites across the country.
However, there is still much more that can be done.
Funding pain management research
For instance, Statistics Canada is mandated to produce statistics on the health of Canadians. Unfortunately, the latest available data on painkiller misuse was released in 2012 (via the Canadian Community Health Survey – Mental Health) and no updated version has been collected since. Scientists across the country are eager to help, but may not have the resources to do so.
Providing national public data repositories would allow researchers across the country to help determine overdose trends, high-risk sub-populations and other important information that could inform national policy decisions and target health responses where they are most urgently needed.
The federal government also has the power to determine which areas of research should be given priority in funding. New initiatives such as the Canadian Research Initiative in Substance Misuse are an important step forward for guiding evidence-based treatments for substance-use disorders.
Priority funding pools could also be set aside to encourage research, education and clinical care targeted toward finding safer pain management approaches — a serious problem that exists for much of the opioid-using population. Currently, there is a concerning lack of evidence-based alternative treatments for chronic pain patients whose opioid prescriptions are being cut off.

All hands on deck
Finally, empowering the health-care workforce to help address the opioid epidemic is essential.
In the United States, nurse practitioners (NPs) and physician assistants (PAs) play an important role. The Comprehensive Addiction and Recovery Act signed by President Obama on July 22, 2016, authorizes qualified NPs and PAs to prescribe medications for patients with Opioid Use Disorder. This provides more than 86,000 extra people who could be eligible to help prescribe life-saving addiction treatments, in addition to physicians.
In Canada, there is not enough recognition of the potential role for nurses and other allied health professionals to help. Allocating funding for more training and staffing for these skilled professionals would promote an “all hands on deck” approach to assessing and treating pain and addiction, administering overdose-reversing interventions, assisting with urgent clinical research and educating and supporting affected communities.
If Canada were to declare a public welfare emergency, more health centres with skilled staff performing these essential roles could be immediately mobilized to help curb the opioid epidemic.
It’s time to recognize the opioid overdose crisis as the national public health emergency that it is.
This piece was originally published at ![]()
![]()