Is this flu season bad? No one knows
Why there is no good measure of influenza virus infections, deaths, and similar respiratory illnesses
Man sneezing at bus stop
Share
There has been plenty of discussion about a particularly bad influenza season in Canada, and even more so in the U.S., as both nations appear to brim with feverish, coughing patients. Things have been so bad south of the border that New York state and Boston declared public states of emergency and the U.S. Centers for Disease Control and Prevention (CDC) said that flu-related deaths have reached into epidemic territory.
But what does that actually mean? According to the CDC, the epidemic threshold for influenza—a virus that attacks your respiratory system, not your guts—is when related deaths account for more than 7.2 per cent of all deaths in a given week. For the week ending Jan. 12, 8.3 per cent of all deaths were due to pneumonia and influenza, just above the epidemic threshold.
This sounds scary, but the death counts from pneumonia and influenza actually aren’t all that high when compared to recent flu seasons. Check out the chart below:
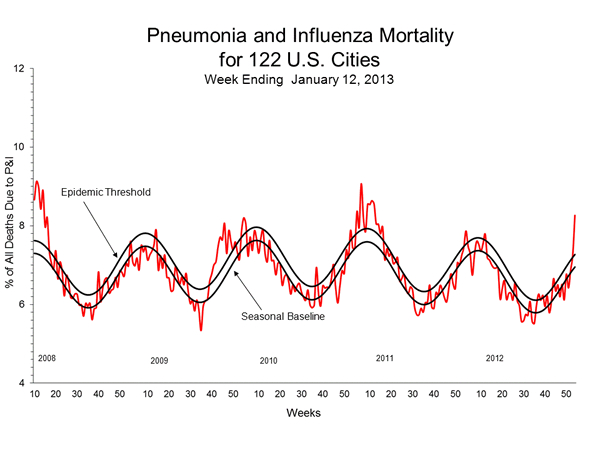 |
“So far the recorded (pneumonia and influenza) mortality is barely above what they call the ‘epidemic threshold,’” said Peter Doshi, a postdoctoral fellow at Johns Hopkins University School of Medicine who has studied influenza mortality, “but there is still time for things to change, of course.”
Though he said he doesn’t doubt hospitals are experiencing a surge this year, he asked: “What is influenza’s role in that? It’s not clear. It could be norovirus, coronavirus, respiratory syncytial virus (RSV), we don’t know.”
The patchy surveillance system for influenza
That’s because, the truth is, no one truly knows how many people actually have the influenza virus, how many people die from it, and how many others have illnesses that are masquerading as the flu. There’s no surveillance system for influenza anywhere in the world, no one tracks flu-related illnesses, and death estimates are mostly based on statistical models, not body counts.
The only way to know whether someone has influenza is to do a lab test. But flu reporting is based on people who happen to be tested since there’s no random sampling of the population. So if most people with influenza-like illnesses don’t go to the doctor or hospital, they are never counted. This means that a lot of folks getting sick this winter may have influenza, or something else. As well, without random sampling, it’s hard to know what the baseline of sick people in a given year actually looked like.
As for flu deaths, Doshi explained, there are the confirmed cases, but statistical models try to account for people who die from a complication due to the influenza virus. For example, deaths from heart attacks brought on by sickness with influenza. But whether or not they actually had influenza is never confirmed. These are best guesses.
Another measure of the severity of the season is pediatric death from influenza. Doshi explained that when an elderly person dies, the cause of death is not always determined. However, pediatric deaths are more unusual and tests to confirm the cause of death in a child are common. As a result, this measurement tends to be more precise than the adult estimates. This year, U.S. pediatric deaths due to influenza are, thankfully, rather low. (So far, 29 this season.) “Right now, for influenza-associated pediatric deaths, it’s the least deadly season since the CDC started recording (these deaths) in 2004/2005,” noted Doshi.
Here are the pediatric deaths for this year, as compared to other years:
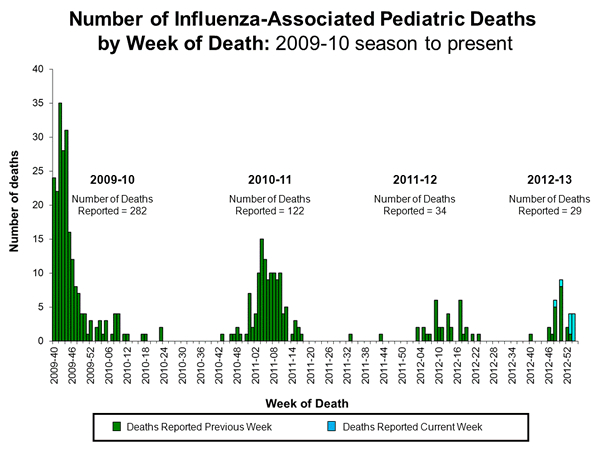 |
The flu situation in Canada
As for Canada, infectious disease expert Dr. Allison McGeer said that the consensus in the medical community is that it’s a busy season, and one that started earlier than usual, “but it’s not out of range.”
Here, too, Canada relies on imprecise statistical modelling to measure flu activity, and McGeer said it will take a year to gather enough data to know how bad the 2012-2013 season truly was. As for confirmed deaths nationally, the Canadian Press reported that there have been 15 in people 20 years of age and older, and no pediatric flu deaths. Still, in any given year, McGeer estimates, “There’s something in the order of five million flu infections in Canada, but we don’t test all those people.”
Why all the fuss about “flu-mageddon” this season?
“Some of this has to do with strategy around releasing vaccines,” said Doshi, “and some has to do with raising awareness to get people vaccinated. Different motivations are going into public health campaigns.”
There’s always an element of uncertainty that comes with the flu and there is no clear pattern from one season to the next. As McGeer put it: “If you’ve seen one influenza season, you’ve seen one influenza season.”
We can’t tell how bad it’s going to be, but McGeer did offer this: “About one in 10 years, we’ll get through a winter, and there’s almost no influenza. About three out of 10 winters, it’ll be a year like this year, busy. The other six will be somewhere in between.”
No matter the severity of influenza that year, public health officials suggest getting the flu vaccine. It doesn’t protect against flu-like illnesses but it does protect against influenza. The next best protection is something that’s almost free and doesn’t require a prescription: hand washing. Lots of it. Officials suggest aiming for five scrubs a day.
Science-ish is a joint project of Maclean’s, the Medical Post and the McMaster Health Forum. Julia Belluz is the senior editor at the Medical Post. Got a tip? Seen something that’s Science-ish? Message her at [email protected] or on Twitter @juliaoftoronto