
Ebola: Everything you need to know

Ebola is:
- A contagious and often fatal viral disease
- Transmitted through contact with the bodily fluids of infected, symptomatic people
- Without any approved treatment or vaccine
- Spreading out of control in three West African countries in an outbreak that began in December
- Responsible for thousands of illnesses and deaths: Get the latest numbers here
- Killing about 50 to 70 per cent of those infected in this outbreak
- As much as 2.5 times worse than current figures show
Read on to learn the basics about Ebola, or click below to jump ahead:
- Ebola treatments new and old
- Mapping the spread
- Why we can blame bats
- The epidemic of fear
- Ebola FAQ : Why health workers are dying, how hip-hop might end the epidemic, and what you can do to help
- More stories from Maclean’s about Ebola
What Ebola is like
Between two and 21 days after getting infected with Ebola, people develop scorching fever, intense weakness, excruciating muscle and joint pain, and occasionally a rash and sore throat. Once they’re showing symptoms, they can spread the disease to others through all the bodily fluids they’re suddenly producing—vomit and diarrhea, often bloody, and sometimes bleeding from their gums, nose and eyes. Contrary to popular belief, Ebola patients do not die from blood loss. Many die despite not experiencing any bleeding at all.
It’s the general profusion of fluids that led one survivor to dub Ebola “the stomach flu from hell,” and it’s also what makes the virus so infectious. Touch the fluids of someone who has it, and touch your own eyes or nose, or a tiny cut on your skin, and you have it too. Men who have been through Ebola may carry live virus in their semen up to 7 weeks after recovery. It also passes into breast milk, but there’s not enough research yet to know if the virus lingers there after recovery. Although some transmission by droplet spray is apparently possible, Ebola mercifully does not hang around in the air like influenza or the common cold. It’s no match for sunlight, household bleach, or even soap and warm water.
Scientists have identified several strains of the virus, including one that doesn’t seem to cause disease in humans, Ebola Reston. This epidemic is caused by a variant of the ultra-deadly Zaire Ebolavirus strain. There are serious barriers to keeping track of the number of sick and dying people. Doctors in the field report that about half of patients who enter treatment are surviving the virus. Where the WHO has been able to definitively track Ebola cases, they’re finding a fatality rate of 70 per cent. It’s been as high as 90 per cent in past outbreaks.
A new paper in the journal Science has analyzed viral DNA from 78 Ebola patients in Sierra Leone and found 300 genetic changes in the virus that are specific to this outbreak. It also traced the strain’s divergence from the central African type of Ebola to around 2004. (Tragically, five of the paper’s authors have since died of the disease).
Ebola is sneaky. It attacks immune cells, repressing the body’s ability to fight it off, and weakens the blood vessels, leading to internal and external bleeding. The causes of death vary from person to person. Some are simply overwhelmed by the virus and the immune response from their bodies. Others seem to die of heart attacks or respiratory distress. Hiccups are a death knell in the Ebola patient; a warning that the diaphragm is quitting. Because more people have gotten sick in the past few months than in all other previous outbreaks combined, some less typical signs have begun to surface. Anecdotally, it’s been observed that some patients develop out-of-whack blood sugar, suggesting Ebola might affect the pancreas.
Ebola survivors carry antibodies against that strain of the virus for life. Some report lingering joint pain and vision problems, but at least one missionary doctor who got the virus in the 1970s is still alive and kicking at age 71.

How Ebola is treated
There’s no proven treatment and no vaccine for Ebola, but simple supportive measures drastically improve survival. Rehydration drinks and IV fluids relieve dehydration, acetaminophen controls fever, and antibiotics kill deadly secondary infections. But in settings without reliable electricity or running water, let alone modern hospital equipment, extreme but potentially lifesaving measures like mechanical ventilation are off the table and might even put health workers at more risk.
There’s also an overlooked factor at play. Without the fully equipped lab and testing equipment that Western hospitals take for granted, health workers can’t pinpoint what’s going wrong with a particular person. If someone’s dangerously low on potassium because of diarrhea, regular IV fluids might not help them. If a patient’s blood isn’t clotting properly, they might be helped by an infusion of platelets. But if doctors can’t run blood work, or don’t have any platelets on hand, there’s not much to be done. No one knows what the mortality rate would be if everyone with Ebola had access to the best care, but there’s reason to believe it could be much lower than it is now. That’s why so many Western countries have been evacuating their sick citizens.
High-stakes experiments
In July, when two American health workers and a 75-year-old Spanish priest caught Ebola in Liberia, they were swiftly given an experimental antibody therapy called ZMapp. The drug was developed in part thanks to the research of Canadian Gary Kobinger at the University of Manitoba. It had never been tried in humans before, and experts didn’t know if it was safe even for healthy people to take. The Americans, Dr. Kent Brantly and Nancy Writebol, recovered after treatment at Emory Hospital in Georgia, near the U.S. Center for Disease Control.
Read more about ZMapp from the CDC here, or see a more technical description here.
An Aug. 29 study reported that 18 rhesus macaques infected with Ebola, the entire study sample, were cured with ZMapp. In humans, the drug’s track record is mixed and there’s no way to say yet if it does any good. Before receiving ZMapp, Dr. Brantly was having trouble breathing and reportedly told a doctor he believed he was near the end. He called his wife to say goodbye. But as the IV infused the medication into his bloodstream, his breathing calmed, and the rash all over his body faded. ZMapp seems to have worked for him almost instantly. On the other hand, the priest, Miguel Pajares, was airlifted to Spain and later died. Predictably, the Internet got angry when a handful of Westerners received a "secret serum" to treat a disease that had been killing thousands of Africans for months. Three Liberian health workers later received the drug; one has since died.
On Aug. 25, Japan came forward to offer an anti-influenza drug called favipiravir for the treatment of Ebola. The manufacturer, a subsidiary of Fujifilm, says it will ship the drug as soon as WHO requests it. A third company, Sarepta, has an untested Ebola drug under development that it will deploy if asked.

The first vaccines
The U.S. National Institute of Health will begin the first Ebola vaccine trials the week of Sept. 1, 2014 using healthy volunteers. The trials will determine if the vaccine is safe and if it helps people generate Ebola antibodies. It doesn’t contain any live virus. Clinical trials of a second vaccine called VSV-EBOV, which was developed and licensed by the Public Health Agency of Canada, have begun. Canada has donated its stock of the vaccine to the WHO.
Scientists’ understanding of viruses and antiviral treatments has exploded in recent years. According to University of Reading virologist Ben Neuman, Ebola might prove fairly easy to treat, as viruses go.
“Ebola looks as if it ought to be treatable,” he says. “We have treatments for other similar viruses, and a lot of things work in the lab. There are research groups being formed. Until now, there hasn’t been much of a financial incentive or a practical reason to do so. It doesn’t make sense to spend millions of dollars developing a vaccine for a disease that until recently had only killed about a thousand people worldwide.”
Where in the world is Ebola?
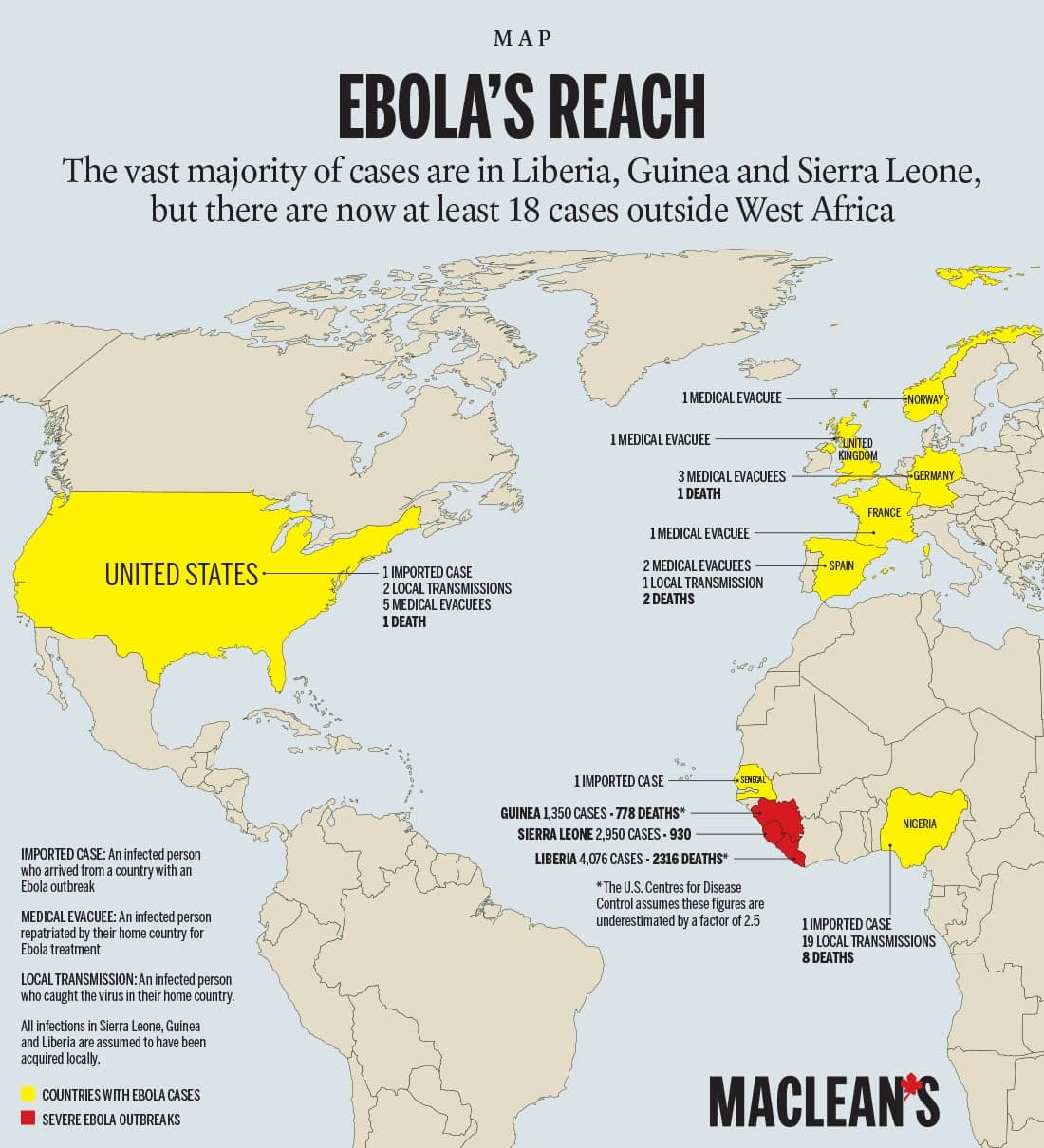
Ebola is spreading uncontrollably from person to person in three coastal West African nations: Guinea, Liberia, and Sierra Leone. A single traveller from Liberia seeded a small outbreak in Nigeria in August; the country has now been declared Ebola-free. A number of other countries have imported cases and limited person-to-person transmission. Two nurses in Dallas, Texas caught Ebola after treating a patient from Liberia who later died. They’re both Ebola-free now.
On Aug. 25, 2014, the Congolese ministry of health announced an unrelated Ebola outbreak in the northern Democratic Republic of Congo. As of Sept. 11, 2014, there have been 66 cases reported locally and 49 deaths. None of the sick people reported travelling to West Africa recently or being in contact with anyone who had. The WHO has traced the outbreak to a single pregnant woman who probably got the virus from an animal that she prepared for cooking. Virological analysis from the WHO has confirmed that the Congolese outbreak is distinct from the West African health crisis.
Blame the bats
The Congolese outbreak is much more typical than the one currently ravaging West Africa. The virus has been playing a grisly game of Whac-A-Mole with public health authorities since it was identified in 1976, popping up most recently in Uganda and the DRC in 2012.
“It’s almost certainly the case that every outbreak starts with the virus jumping from an animal to the human population,” says Harvard virologist James Cunningham.
Most of the time, Ebola lingers quietly in fruit bats that make their homes all across Africa. They’re the suspected natural reservoir—they don’t get sick, but they do harbour the virus. Monkeys and chimps become ill with Ebola just like humans do. In a vast region where millions of people rely on wild game for a cheap, tasty and plentiful source of protein, it’s inevitable that once in a while a human hunter comes into contact with the virus.
“You can find lots of virus in bat caves in the feces. Most fruit bats have antibodies from the (Ebola) virus,” says University of Reading virologist Ben Neuman. “There’s no reason it couldn’t happen anywhere in the region.”
A paper in the New England Journal of Medicine identified the first patient in the West African outbreak as a two-year-old from southeastern Guinea, near the borders with Sierra Leone and Liberia. Researchers speculate the toddler, who died on Dec. 6, may have eaten some fruit contaminated with infected bat feces.
Learn why bats are so good at incubating deadly viruses (Video by Minute Earth):
The epidemic of fear
An evil genius couldn’t have designed a better political and social context for the spread of disease than Liberia, Sierra Leone and Guinea, three of the poorest and most poorly governed countries on Earth. An atrocious war laid waste to infrastructure in all three countries in the 1990s and early 2000s, leaving PTSD, former child soldiers, amputees and rape survivors in its wake. Over the last decade a fragile peace has settled on the region, allowing it to take a third-class ride on the continent-wide economic boom. Rapid urbanization, porous borders and a booming mineral sector have created massive movements of people—desperately poor, barely educated people with a justifiable lack of trust in institutions.
It’s the ultimate incubator for misinformation and half-truths. The most potent and widespread rumour is the idea that Ebola kills everyone who is infected, says Arthur Pratt, the national coordinator of the Sierra Leone film council and director of public service announcements about Ebola. That belief is at the heart of the pervasive stigma against Ebola survivors and families of the sick, and what causes people to hide ailing or deceased loved ones. It also motivates people to seek traditional treatments and religious healers instead of going to the hospital. Why go there, and die alone surrounded by people in space suits, when there’s no hope of recovery? And guilting the sick into self-isolating isn’t going to work in a population where understanding of contagious diseases is low.
Ebola had never hit West Africa before, and fear of the unfamiliar helped far-fetched conspiracy theories take hold and spread, both on the street and on social media platforms like WhatsApp. Claims that Ebola is a cover for organ trafficking, a plot to thin the population, or a way for foreigners to try out experimental drugs and make money will all sound familiar to people who remember stories that circulated about HIV/AIDS decades ago. In Sierra Leone, many people believe the government is trying to exterminate people in the worst-hit area, which happens to be a stronghold of political opposition.
There’s one large and growing group of people who are even more responsible for the spread of disease than rumour-mongers: the dead. The body of an Ebola patient, seeping with infected fluids, is a weapon of mass destruction. A single traditional funeral, where mourners come from far and wide to touch and kiss the body in farewell, can seed dozens of new cases. The women tasked with washing and laying out the body for burial are at greatest risk. The WHO estimates 60 per cent of Ebola cases in Guinea can be traced directly to funerals. The outbreak of the disease in Sierra Leone began when a group of women attended a funeral for a traditional healer who had been treating Ebola patients over the border in Guinea.
In some areas, such as Monrovia, the capital of Liberia, local authorities are having trouble safely handling all the bodies of the deceased. There have been reports of people putting bodies (some with Ebola, others not) out into the streets to avoid having their households quarantined.

What’s being done
On Sept. 30, the United Nations announced a dedicated mission for Ebola emergency response, to be headquartered in Ghana. President Obama has sent thousands of troops to the region, mainly to Liberia, where they are setting up field hospitals, providing logistical support, and training workers.The international community is waking up to the crisis. The WHO and leaders of the three affected countries have announced a joint response plan, and on Aug. 28 the global health authority released a roadmap for ending the outbreak. As with so many diseases, the prescription is money: money for isolation beds, for health worker salaries, for laboratory resources, for infectious disease specialists, for gloves. Money for education campaigns and money for "contact tracers" who track down people who have been exposed.
Canada has donated money and medical supplies, as well as experimental vaccines, to help fight the outbreak and advises against all non-essential travel to the area. The national public health agency, stressing that the risk to Canadians is miniscule, has asked Canadian border officials and family doctors to keep an eye out for people who may have been exposed.
Doctors Without Borders (Medicine Sans Frontiers, or MSF) has taken on a huge portion of the medical and psychosocial care of people with Ebola. It has more than 300 international staff working in the affected countries and admitted thousands of people to its Ebola field hospitals since March. In late August, the organization opened a 180-bed Ebola treatment centre in Monrovia; a week later it was full. The organization estimates that the hospital needs 800 beds to meet the community’s needs. The MSF president says they’re stretched to the breaking point and called on WHO to step in. The Red Cross is also on the ground, providing various auxiliary services, logistical support and disease surveillance in the outbreak zone.
Ebola FAQ, as paraphrased from real tweets and online comments
Q: Ebola spreads through contact with bodily fluids? If doctors in Haz-mat suits are getting it, then isn’t there something they’re not telling us?
No, there’s not. Health care workers are dying in droves because they’re overtired, overworked and overwhelmed. Wearing a plastic body suit, rubber gloves and boots, a face mask and goggles is incredibly oppressive and uncomfortable at the best of times. In the humid, tropical conditions of the West African summer rainy season, it’s unbearable. No one should spend more than a couple of hours at a time in personal protective equipment to avoid dehydration and exhaustion, but many health workers are spending much, much longer than that. And because they’re in close contact with sick people every day, all day, there are infinite opportunities to slip up. A dearth of proper equipment and adequate training is adding to the problem.
Setting up a working isolation ward that separates suspected cases from confirmed cases from the rest of the hospital population is a logistical challenge to which many West African institutions can’t rise. To give just one example, this New York Timesvideo shows the highly infectious body of a person who died of Ebola being carried through a public clinic.
The head of the World Health Organization says a ward with 70 Ebola patients needs 250 health workers to operate safely. Some hospitals, understandably, are having a hard time getting anybody to show up for work. Take the case of William Pooley, a 28-year-old British volunteer nurse who contracted Ebola in Kenema, Sierra Leone, and had to be airlifted out. He told a local journalist before he got sick that he and the head nurse had to leave the isolation ward completely unattended overnight after it was the site of a violent protest. They were the only two people there to care for 45 patients, and they left knowing they’d find bodies in the morning.
That type of situation inevitably worsens the spread of disease. The widespread rumour that the virus is spreading through the air is completely unsubstantiated. Ebola only spreads through contact with infected bodily fluids. But it only takes a tiny dose to get infected and get sick. Yes, all viruses change and mutate—that’s why some flu seasons are terrible and others mild. Theoretically, the Ebola virus could mutate and become airborne. But just because it’s possible, doesn’t mean it’s likely. If you could get Ebola by breathing the air near an infected person, the WHO and CDC would be warning people to wear masks in affected areas at all times.

Q: I can’t believe they’re bringing infected people to this continent to be treated. Aren’t we in for a global pandemic?
That’s highly unlikely. It takes close personal contact with an infected and symptomatic person to catch Ebola, and once you’re ill, you can hardly move. Most of the sick people are very poor and unlikely to get on a plane, and even if they did, the world is on high alert for travellers from West Africa who look even slightly peaky.
The negative pressure units and Haz-mat suits that Western countries deploy to evacuate infected citizens are scary-looking and might seem excessive for a virus that is only moderately contagious. In fact, they are excessive. But it’s not often that public health agencies get to use these toys outside of the lab, and there’s good reason take every affordable precaution. Once infected, even the healthiest person has a high chance of dying from Ebola.
Q: How come only a handful of people received the experimental drug? Why don’t we try it out on everyone? There’s not much to lose.
There’s not much to lose. That’s what the World Health Organization says, too. The agency convened a panel on the ethics of using untested therapies, and decided that the risk is worth it as long as research subjects can freely choose to participate or not, understand the risks and benefits, and are carefully studied. Unfortunately, the last known doses of ZMapp, one of the only experimental drugs ever tried for Ebola, are all gone now. It’s going to take a while to make more. Expect more news about vaccine and drug trials in the coming weeks.
Q: Everyone’s overreacting to Ebola. Look at all the people who have died of (TB, HIV/AIDS, malaria, cholera, etc.) since the outbreak began.
Even without Ebola, drastically underfunded local hospitals nearly drown every summer as the rainy season brings waves of cholera and malaria. As health care workers are felled by the virus, health centres are commandeered for Ebola patients, and families choose to keep sick loved ones at home rather than risk being infected, more people will die preventable deaths from common ailments. That’s why it’s essential to get this outbreak under control.

Q: People won’t accept treatment because they don’t know what Ebola is, or they don’t believe it exists. What’s the point?
Ignorance and misinformation are certainly obstacles. But people can change their minds. Hip-hop stars—pop-culture royalty in West Africa—have churned out dozens of educational tunes to spread the word about the outbreak. The top track in Liberia right now is the catchy "Ebola song"; other favourites include “State of Emergency” and “Ebola in town” (lyrics: "Ebola in town / don’t touch your friend / no kissing!"). Liberian soccer-star-turned-politician George Weah recorded an educational ditty called "Ebola is real."
Listen to the UNICEF-sponsored "Ebola song":
Local organizations like the Boy Scouts are helping spread awareness, and in Sierra Leone a series of public service announcements such as this one made by the NGO WeOwnTV are being shared on the Internet and played in public spaces. (Warning: the video is designed to educate people who may not be literate. It contains a rather convincing demonstration of what bloody vomiting looks like.)
Finally, the growing group of Ebola survivors—who understand the virus, have seen the inside of isolation wards, and lived to tell about it, are helping to correct misinformation in their communities and calm the paranoia surrounding the disease.
To answer the question: The point of the effort is to stop the spread of Ebola now, using public health measures. If that doesn’t happen, there’s a risk it could become endemic in West Africa, meaning it never fully goes away, adding to the already-heavy disease burden and hampering the whole region’s economic and social development.
Q: Why don’t we just wall off this entire region and cease all travel in and out? Desperate times call for desperate measures.
There’s no evidence that works. When local police enforced a blockade of West Point, a slum neighbourhood and Ebola hotspot in Monrovia, Liberia, violence erupted as fears of the disease and of starvation spread. The quarantine is fairly easy to get through, if you have a little money for a bribe, and people got to from work from West Point by swimming along the coast.
Restricting access to Ebola-affected regions makes it harder to get food and supplies where they need to go. The price of staples is skyrocketing, and the World Food Programme has had to step in to fill the need.
The WHO does not recommend border closures or travel restrictions, except for people who are showing signs of Ebola or have been in contact with someone who has.
Q: How can I help?
If you want to give money, Doctors Without Borders (MSF) is providing direct care to people with Ebola. The Red Cross and Plan Canada are both leading public education campaigns. If you can give your time, the United Nations has urgently appealed for doctors, nurses, and other health professionals to come forward and volunteer.
Read more from Maclean’s about Ebola
Get the Best of Maclean’s straight to your inbox.
Sign up for news, commentary, analysis and promotions. Join 80,000+ Canadian readers.