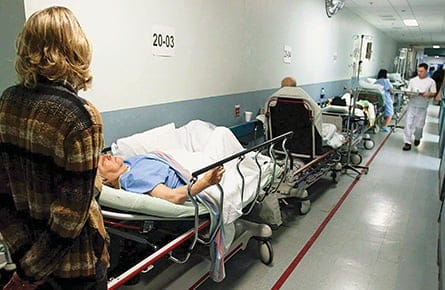
When it comes to waiting for health care, Canada is last in line
Wait for the next available customer service agent. Wait for your boarding call. Wait for the ads to end so the movie finally begins. Waiting is a major component of modern life. And while most of that time spent waiting is simply an inconvenience, sometimes it can be life-threatening.
For decades, wait times have been a consistent and much-lamented component of the Canadian health care system. Within the strictures of medicare, we endure lengthy waits for family doctors, specialists, tests, therapy, beds and on and on. Canadians, in fact, wait longer and more often for health care than citizens in all other developed countries. Why do we consider this acceptable?
Earlier this month, the Organisation for Economic Co-operation and Development (OECD) released a major survey on international health care waiting lists and policies. Canada is at the bottom of the pack in almost every category. One example among many: 25 per cent of Canadian patients waited more than four months for non-emergency, elective surgery, the highest proportion of any country reported. The figure is 18 per cent in Australia and seven per cent in France, Switzerland and the United States.
The OECD also reveals Canada to be one of five countries (out of a survey of 22) that report major wait-time problems in all six possible health care categories—from emergency rooms to long-term care.
Finally, and perhaps most depressing, we’re included in an unhappy group of counties that spend above the OECD per capita average on health care but nonetheless report significant wait times. We pay more but still underperform.
To be fair, Canada has made substantial progress on wait times over the past decade. But this just reflects the depth of our problems. A major federal-provincial agreement in 2004 allocated more money and attention to waiting lists, designating five priority areas for wait-time reductions—cardiac, cancer and cataract care, hip and knee replacements and diagnostic imaging—and setting benchmark times for treatment. It also committed to greater transparency about how long Canadians wait.
Since then, all provinces have put wait-time data online for everyone to see. And measured by the benchmarks, waiting has generally improved across the five priority items. Ninety-nine percent of all cardiac patients, for example, now receive bypass surgery within the specified time frame. (Although anyone with a heart problem might argue that six months is a rather generous benchmark.)
Without question, all this scrutiny has improved health care provision in this country. And with the 10-year 2004 agreement set to expire next year, Canadians are being told a story of great progress. But we still wait much longer than our peers in other countries. We can do better.
Certainly, a broader array of services needs to be included in any new deal, one that covers the more routine aspects of health care, such as emergency-room, rehab and long-term care. According to a survey of 11 developed countries, Canadians make the most use of emergency departments and are most likely to wait longer than four hours to see a doctor.
Canada should apply successful strategies from other countries, regardless of ideology. “High expenditure is not a guarantee of [short] waiting times,” reminds the OECD report; evidence-based innovation is more important than money. That countries with public health insurance and no patient cost-sharing tend to have the longest waiting lists suggests Canada’s sacred medicare system may be one of the biggest obstacles to improving service. Finland, for example, found that a voucher system for certain procedures led to a reduction in wait times. It also established wait-time guarantees (as opposed to benchmarks) enforced by fines.
We need to take note of innovations occurring within our own borders, as well, such as successful pay-for-performance experiments in British Columbia and dedicated nursing-home paramedics in Nova Scotia whose goal is to reduce the number of ambulance trips taken by seniors. St. Mary’s General Hospital in Kitchener, Ont., even posts up-to-the-minute emergency-room wait times on its website (6.5 hours to see a doctor, as of noon on Monday), allowing potential patients to make informed decisions on their best treatment options. From this perspective, the recent news that, for political reasons, Quebec has dropped out of a pan-Canadian committee on health care innovation seems entirely retrograde.
However much progress Canada has made to date on health care wait times, the fact remains that we’re still worst among our peers. A real and permanent solution will require focus, imagination and an end to misplaced ideology. There’s no time to waste.
Get the Best of Maclean’s straight to your inbox.
Sign up for news, commentary, analysis and promotions. Join 80,000+ Canadian readers.