Hospital performance is all over the map
Quality of care varies from province to province and hospital to hospital, according to newly released data
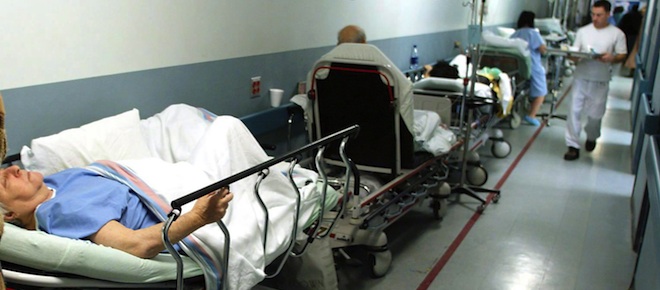
Patients line up on hospital beds outside the crowded emergency room at Montreal’s Sacre Coeur Hospital Thursday, Nov. 28, 2002.A new report says health-care costs in Canada doubled over the past decade and will cross the $200 billion mark this year. THE CANADIAN PRESS/ Paul Chiasson
Share
It’s long been a truism of the Canadian health care system that where you live determines the kind of care you receive. Large hospitals in growing urban centres tend to have more resources and equipment than smaller rural hospitals with remote and ageing populations.
But a new project tracking the performance of the most of the country’s hospitals – the first ever publicly released in Canada – shows just how much where you live might make a difference in how likely you are to survive a heart attack, stroke or major surgery, or whether you’re more likely to give birth naturally or by cesarean section.
The hospital reporting project, released today by the Canadian Institute for Health Information, compares 600 of the country’s hospitals, more than half of which are small community health centres, on a host of issues, such as deaths in hospital after strokes and major surgery, trauma from giving birth, and how much of a hospital’s budget goes toward its administration costs instead of patient care.
For example, you have a 40 per cent greater chance of dying in hospital of a heart attack or stroke in Newfoundland than in Saskatchewan or Alberta, but you’re more than twice as likely to die within days of a major surgery in Saskatchewan than in Prince Edward Island. You stand nearly double the chances of suffering what hospitals call a “nursing related adverse event” such as a bedsore, in Nova Scotia than in Prince Edward Island.
Alberta has the lowest wait times for surgery for hip fractures, with nearly 83 per cent of patients being treated within 48 hours of breaking their hips, compared to 76 per cent in Saskatchewan.
There are also dramatic differences among hospitals in the same province. In Ontario, for instance, 30 out of every 100 stroke patients died in Brockville General Hospital, compared to fewer than 9 of every 100 in The Scarborough Hospital in Toronto.
Overall, hospitals have been getting safer and patients more likely to survive major illnesses and medical procedures. But there are still unexplained differences between the hospitals that are leading the country and the ones that are struggling.
“We’re seeing that hospitals are moving in the right direction,” said Jeanie Lacroix, manager of hospital reports at CIHI. “But we’re still seeing the variation that we’ve seen for many years and we need to assess why that’s still happening.”
Among the most striking differences are the rates for cesarean sections for low-risk pregnancies, a measure that matters because cesarean are both more expensive than natural births and harder on both the mother and the child.
In Manitoba, 21 per cent of low-risk births were performed by c-section compared to 33 per cent in Newfoundland. At the hospital level, the range was even greater: At Burin Peninsula Hospital in Newfoundland, 47 per cent of births were by c-section, compared to just 2.45 per cent of births at Slave Lake Healthcare Centre in Alberta.
The amount of money spent on both administration and patient care also varies between provinces. Newfoundland had the highest costs per case of the provinces, at nearly $6,250 per patient, or about 20 per cent higher than the Canadian average of $5,167. Costs have been going up across the country, up 1.3 per cent in 2009 and 3.4 per cent in 2008.
The proportion of hospital budgets that gets spent on administration has gradually been dropping, but was highest in Ontario, where $1.12 billion, or nearly six per cent of overall expenses, went toward administration costs. That’s nearly double the 3.5 per cent spent in Alberta.
The report comes at a time when hospital executive compensation has been under intense scrutiny in Ontario as the minority Liberal government heads into its first post-election budget.
Mark Rochon, head of the Ontario Hospital Association, questions just how much the hospital spending can be compared between provinces, since Ontario has 150 separate hospital corporations, each with their own CEO and executives, while Alberta has a single health care administrator.
“The issue for us is whether we’re truly comparing apples to apples when we look at Alberta versus Ontario,” he says.
Ontario’s per capita health spending is $300 below the national average and well below what Alberta spends. Still, he says, there are benefits to studying a system like Alberta, with fewer hospital CEOS and more centralized administration.
“If there is an opportunity for us through different organizational relationships to improve the performance of the heath care system in Ontario, then we’re for it.”
Ontario Health Minister Deb Matthews said the province has no plans to move toward more centralized hospital administration, which has seemed to cut down on administration costs in Western provinces.
“I think a community voice at the table is important,” she says. “[Hospital boards] raise a lot of money for their hospitals. They do bring a lot of value to the communities. So we have no plans at all to move toward taking over all the hospitals.”
Ontario’s high administration costs are largely a byproduct of an increasing array of hospital reporting requirements being handed down from the province that forces health care centres to hire legions of managers and executives rather than doctors and nurses, says Natalie Mehra, executive director of the Ontario Health Coalition, an advocacy group.
“The administration office used to be a suite of offices in the hospital building,” she says. “Now they have whole separate buildings used for administration and hospitals will say, fairly so, that this is not their fault. That they’re required to report on more and more and more things and that’s true in Ontario.”
“It’s a very technocratic approach to health care that this government has and it’s led to the elevation of the whole managerial class of technocrats and consultants and review after review after review of the same thing. It’s really unpopular with the public.”
Meanwhile, officials in Prince Edward Island were getting set for damage control after the hospital tracking project reported that the province’s Health PEI spent nearly 16 per cent of its budget on administrative costs.
Executives said the number was a data entry error and that their administrative costs were around 4.7 per cent of their budget. CIHI said its data on Health PEI was “under review.”
“If 16 per cent of our total health care budget was spent on administrative costs right now my job would be a lot easier,” says CEO Keith Dewar. “It’s really three times the amount we’re spending on administration. We couldn’t sustain it right now. We’re not allowed to do that and I don’t know what we’d do with all of those resources.”