Should we make surgeons get tested for HIV, hep B and hep C?
Science-ish looks at the evidence on infected doctors
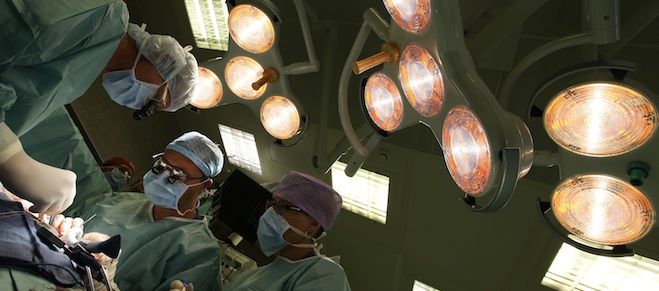
Professor Jan Pirk (L), doctor Marian Urban (C) and suture nurse Diana Vapenkova perform a heart surgery at the Institute of Clinical and Experimental Medicine (IKEM) in Prague, June 28, 2012. A Czech medical team led by Pirk has performed a breakthrough operation on a 37-year-old heart failure patient, replacing his heart with two mechanical blood pumps, HeartMate II. The man is the first to survive such surgery, which was performed on April 3. The exact operation was previously conducted by heart surgeons in Texas, United States. However, the patient died one week later. Picture taken on June 28, 2012. REUTERS/Petr Josek (CZECH REPUBLIC – Tags: HEALTH SCIENCE TECHNOLOGY SOCIETY)
Share
When patients go into the hospital for a surgery, it’s next to a miracle they ever leave the building unscathed. It’s not that hospital administrators and health professionals don’t do their best to protect patients—they do. But with the incredible complexity of surgeries and modern hospital systems, the intricate pathways of care, there are infinite possibilities for things to go wrong.
In the media, we tend to focus on the risks related to hospital-acquired infections or the wild pre-checklist days. But there’s another danger that isn’t talked about much outside of medical circles: getting a blood-borne infection, such as HIV, hep C and hep B, from your health-care provider.
Precautions are taken at every turn to make sure diseases aren’t transmitted from doctor or nurse to patient—and vice versa. And the risk of transmission is remote. Extremely, utterly, almost infinitesimally remote. To give you a sense, according to the U.S. Centers for Disease Control, the occupational risk of infection with hep C after a needlestick injury or cut is less than two per cent. That’s somewhere between the risks related to HIV (less than one per cent) and hepatitis B (six to 30 per cent, though surgeons working today would be vaccinated for hep B).
In Canada there have been no documented cases of physicians transmitting hep C or HIV to patients since modern antiviral therapies came on the scene to treat blood-borne pathogens and doctors started implementing what’s known as “universal precautions”—or avoiding contact with patients’ bodily fluids by using gloves, gowns and masks. There has been one reported case of hep B transmission, but it occurred before antivirals and universal precautions. Worldwide, the documented number of health-care worker to patient transmissions of blood-borne infections since 1991 has been “exceedingly low.”
Yet, provincial medical regulators in Canada are targeting blood-borne pathogens in surgeons. The College of Physicians and Surgeons of Ontario just introduced a new policy that asks surgeons—and those who assist in surgery—to report if they have been tested for the blood-borne pathogens hep B, hep C, and HIV in the last year.
Why are they doing this? According to CPSO council president Dr. Robert Byrick, because “physicians were not testing regularly when only the ethical obligation was presented to them.”
As I wrote in a magazine feature for Maclean’s last week, doctors don’t like this policy. “We’re very skeptical of the change,” said Hamilton, Ont. surgeon Dr. Andre Lamy. Not only is the requirement an infringement on his individual rights and privacy, he said, but there’s little science to back it up. “In the last 10 to 15 years, there’s no evidence that shows patients are at risk.” Even the CPSO acknowledged that “the appropriate frequency of testing was uncertain.” A number of health-related bodies—including the Canadian Medical Association, and the National Institutes of Health and the Centers for Disease Control in the U.S.—recommend against mandatory testing of doctors. In addition, it’s well-known that health-care workers are at a much greater risk of exposure to blood-borne disease than patients. Does this mean all patients should be screened? What would be done with the sick ones?
For surgeons who test positive and may have to stop working, there’s little support in place. As Dr. Lamy put it, “If I get infected, will the college take care of me? The answer is no.” He continued: “I would have to quit practicing. I don’t know what I would do.” That’s why some observers note that asking doctors to report on their health to their licensing bodies may actually encourage mis- or under-reporting.
Still, should medical regulators ignore the risk—however small—that infected doctors and nurses pose to patients? We know that health-care workers do sustain needle-stick injuries at work. According to one study of U.S. teaching hospitals in 1990, injuries happened in 6.9 per cent of the surgical procedures examined. As well, the sharp object that injured the surgeon went back into patients’ wounds in 32 per cent of cases.
That’s why there’s near universal agreement that surgeons specifically—along with other health-care providers who face similar occupational hazards—should know their serological status for their own health and the health of patients. As Dr. Mary Vearncombe, medical director of infection prevention and control at Sunnybrook Health Sciences Centre, explained: “If they are positive for any one of those pathogens (HIV, hep B, or hep C), they should seek guidance with regard to their practice in terms of minimizing any possible risk to the patient. There are things you can do in terms of how you practice to minimize risks—like double-gloving and managing how you handle sharps.” Yet, according to at least one medical regulator (the CPSO), surgeons aren’t voluntarily lining up to be screened. In fact, according to some of the surgeons Science-ish spoke to, they are downright avoiding it.
So this raises the question: is there a better way to manage the risks related to transmitting blood-borne pathogens to patients in the operating room?
Dr. John Haggie, president of the Canadian Medical Association, thinks it makes sense to set-up up a fund—a sort of insurance—to protect doctors who need to step away from the scalpel because of an infectious disease. This would mean they wouldn’t be left to choose between their livelihood and their health as well as that of their patients.
From the patient’s perspective, Sholom Glouberman, president of the Patients’ Association of Canada, suggested that, in the name of informed consent, we ask infected doctors to disclose their status to patients and leave it up to them to choose whether to go under their knife instead of leaving decisions about who can practice to the colleges. The risk of infection is so remote, he added, “If it’s a doctor the patient knows and trusts, they would probably prefer to continue to see him or her, rather than going to someone else.”
The other option would be to follow Quebec’s lead. The Quebec college does not mandate screening of doctors because, they say, it’s “medically unnecessary and potentially harmful.” But if physicians who get screened test positive, they go to the Blood-Borne Infection Risk Assessment Unit. There, scientists making evidence-based decisions—independently from the college—figure out the best course of action for infected doctors, free from the legal considerations provincial medical-regulators face.
Another good idea would be to standardize policies around how infected surgeons are treated by the colleges. At an annual meeting of provincial medical regulators in June, Science-ish learned that infected doctors across this country have been managed quite variably, and that there are also regional discrepancies in policies regarding blood-borne pathogens. If processes were more clear and transparent, maybe surgeons would be less afraid to disclose their status, or at least get tested.
In their healing work, physicians have also been vectors for disease, sometimes acquiring infections on the job. It’s an occupational hazard. But we’ve come a long way since the days before hand-washing or even the early hours of AIDS, when it was known as Gay-related immune deficiency disorder. College policies should reflect these advances in science, or figure out how to protect doctors who test positive in mandatory screening.
QUIZ:
Would you go under the knife of a surgeon infected with HIV, hep B, or hep C?[polldaddy poll=”6400635″]
Science-ish is a joint project of Maclean’s, the Medical Post and the McMaster Health Forum. Julia Belluz is the associate editor at the Medical Post. Got a tip? Seen something that’s Science-ish? Message her at [email protected] or on Twitter @juliaoftoronto